Inhalation therapy using a nebuliser – Instruction Video
Medications delivered via a nebuliser for bronchiectasis:
Isotonic saline 0.9%
Hypertonic saline 6% – 7%
Antibiotics e.g. Colistin, Tobramycin
Bronchodilators e.g. Atrovent, Salbutamol
Nebuliser recommendations (ERS Guidelines 2001):
Choose a nebuliser based on the recommendations for the drug that is being prescribed
Choose a compressor that has been tested with the prescribed nebuliser brand
Instruct patients re correct use of the device and the cleaning procedure
Instruct patients that they should follow the manufacturer’s recommendations for when to purchase a new nebuliser
Nebuliser technique: see Nebuliser Therapy video
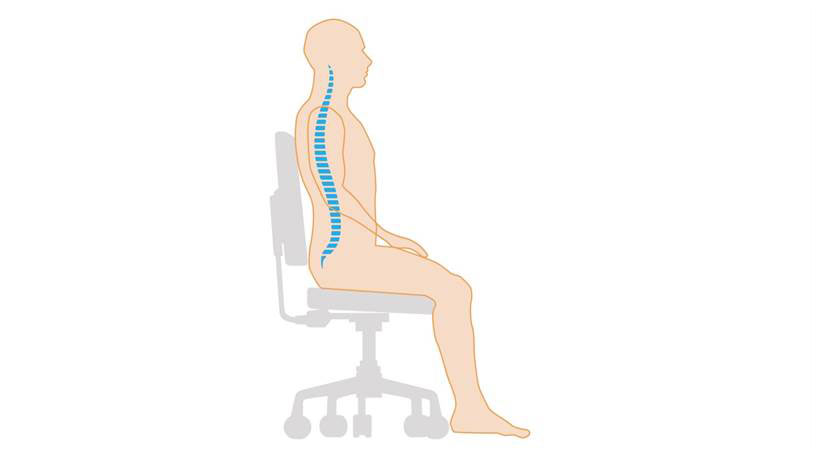
Sit in a well-supported chair with a neutral lumbar spine – this enhances the function of the diaphragm and the pelvic floor and minimises musculoskeletal stress (Fig. 1)
Use a mouthpiece *, if possible, and place it well into the mouth on top of the tongue
Instruct the patient to breathe in slowly, with varied inspiratory volumes
Hold the breath briefly before exhaling
Continue until the nebuliser bowl is empty
* A mouthpiece should always be used unless:
Only masks are provided by the hospital or clinic
The patient is physically or cognitively not able to manage a mouthpiece
The targeted area for deposition is the sinus region
The benefits of the inhaled delivery of medications via a nebuliser are:
Reducing the dose to the body and the systemic side effects
Direct delivery of an aerosolised medication to the smaller airways
Ability to humidify the lower and upper airways
The optimal system should be selected for each individual depending on:
The medication prescribed
The targeted site of deposition eg bronchioles, sinus region
Patients physical and cognitive ability
Financial constraints
Need for portability eg travel
A common clinical problem is that patients are prescribed a medication requiring a nebuliser but the nebuliser is not prescribed.
An inefficient nebuliser may considerably decrease the respirable dose by up to 10-fold (Boe 2001).
Table 1. Nebulisers recommended for people with bronchiectasis who benefit from a small aerosol particle-size to target the peripheral airways.
| PARI Sprint Star – (with red insert) |  | Total Output Rate: 450 mg/min MMD(mass median diameter):2.2µm Mass percentage below 5µm: 89% | When used with Pari SX compressor. Fine particle size for targeted delivery to the peripheral regions of the lung. |
| PARI Sprint – (with blue insert) |  | Total Output Rate: 590 mg/min MMD(mass median diameter):2.9µm Mass percentage below 5µm:75% | When used with Pari SX compressor. |
| InnoSpire Deluxe compressor |  | MMAD – 3.4 µm Fine particle fraction – 67% below 5µm Weight – 2.2kg | To be used with the SideStream Re-usable or SideStream Plus nebulisers. |
| PARI Boy Classic compressor |  | Warranty: four (4) years Power supply: 230V~ 50/60Hz – 0,7 A – 80 W Dimensions: W 19,2 x H 14,5 x D 15 cm Weight: 1.7 kg | Replace filter every year. Service when pressures significantly fall below 1.5 bar. |
| PARI Sinus (compressor can also be used with Pari Sprint and Sprint Star) |  | Total Output Rate: 220 mg/min MMD(mass median diameter):3.2µm Mass percentage below 5µm: 71% | Pulsed aerosol delivery to the nasal cavities |
| Bird e-Chamber |  | MMAD of 2.5µm – 4.5µm Nebuliser rate of 0.3ml/min – 0.7ml/min | Portable light weight nebuliser. Only suitable for nebulised saline and hypertonic saline. |
| PARI eFlow |  | Total Output Rate: 500 mg/min MMD(mass median diameter):4.1µm Mass percentage below 5µm: 64% See Technipro Pulmomed video for use and care of this device: http://www.pulmomed.com.au/eFlowrapidvideo.html | Max fill volume – 6mls Weight – 300gms |
| Flaem NebulAir+ compressor |  | MMAD: 2.21µm Fine particle fraction: 84.2% below 5 µm Weight: 2.4 kg Warranty: 3 years Made in Italy | When used with Flaem RF7+ nebuliser Heavy duty compressor for continuous use Capable of producing up to 14 L/min of flow |
| Flaem RF7+ nebuliser | 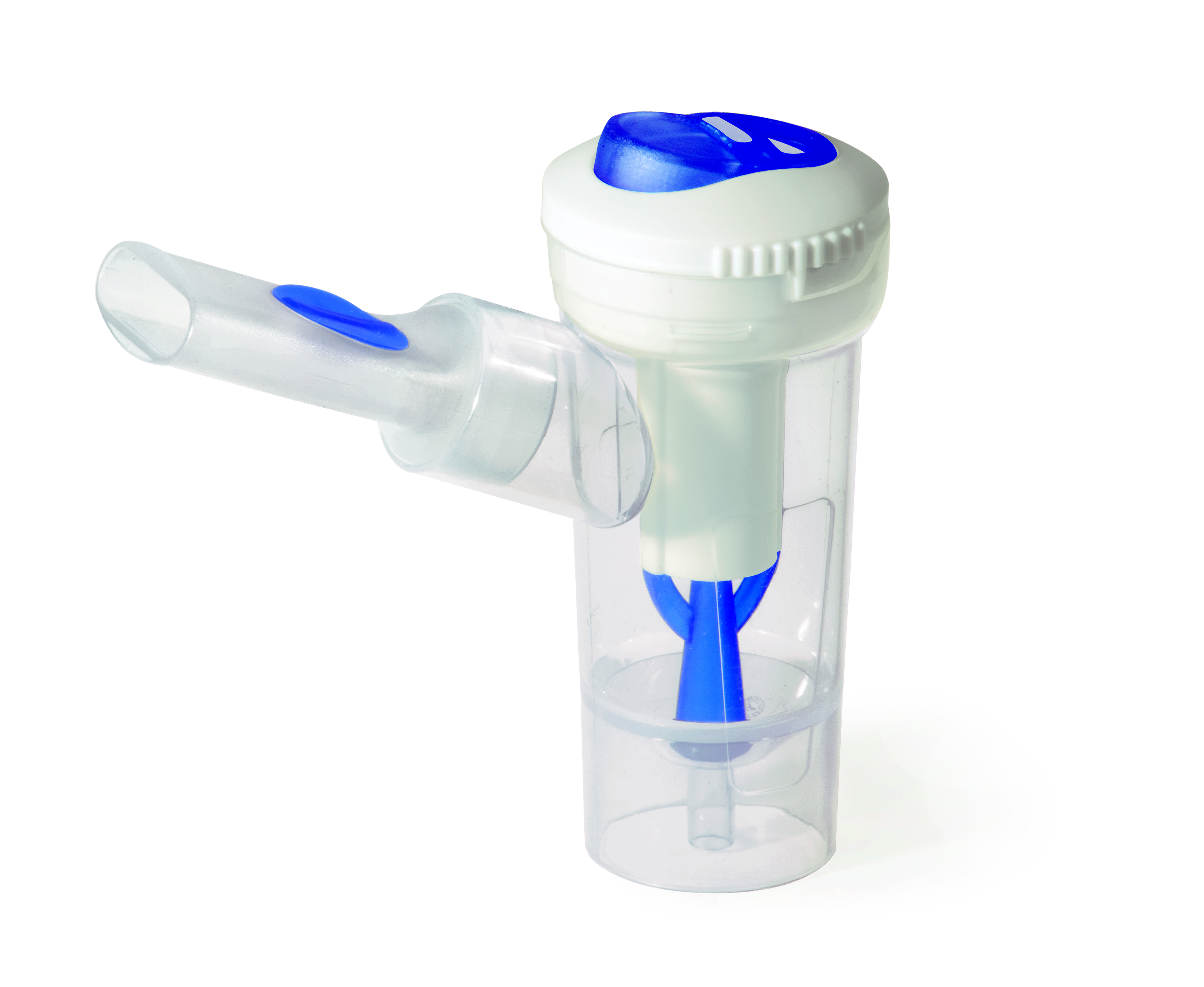 | MMAD: 2.21µm Fine particle fraction: 84.2% below 5 µm Can be used with any nebuliser compressor Dual speed valve to select between faster treatment or maximum drug delivery | When used with Flaem NebulAir+ compressor |
| Flaem RespirAir compressor |  | MMAD: 2.53µm Fine particle fraction: 79.6% below 5 µm Weight: 1.45 kg Warranty: 3 years Made in Italy | When used with Flaem RF7+ nebuliser Compact, sleek and powerful with high quality ABS polymer finish capable of producing up to 10 L/min flow |
For further information on these nebulisers:
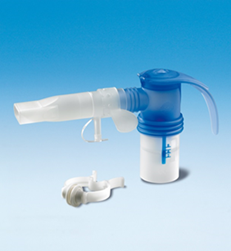
InnoSpire Deluxe compressor and SideStream nebuliser
The compressed air supplied by the compressor passes through the nebuliser nozzle and creates the aerosol at the nozzle outlet (Fig.2). The aerosol thus created can then be inhaled using the mouthpiece or a mask.
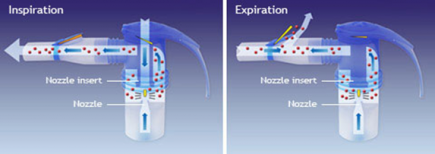
Fig. 2 Production of aerosol
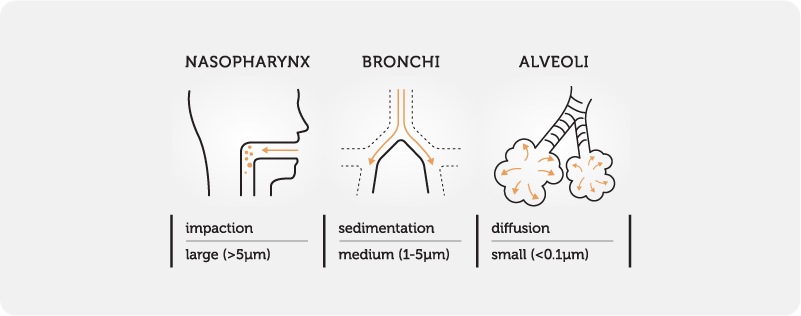
The main factors which determine where in the respiratory tract a nebulised drug droplet will deposit are:
Droplet size (see Figs. 3&4)
Ventilatory pattern
Age and/or condition of the lung
Temperature and humidity
Gravity – deposition is greatest at the bases in sitting, side lying may increase apical deposition
Larger droplets can deposit by impaction on airway bifurcations
Smaller aerosols deposit by sedimentation and diffusion in the smaller airways and alveoli

The ventilatory pattern also effects deposition (see technique, above). The PARI PIF (Peak Inspiratory Flow) system (found in PARI nebulisers) provides feedback to patients on the correct breathing pattern. Resistance is felt on inspiration if the flow rate is too high (above 25L/min).
Additional information when using a nebuliser:
Cleaning of all nebuliser equipment is essential and should be done daily to prevent infection. See manufacturer’s instructions for the correct procedure for each device.
Cleaning all PARI nebulisers and accessories:
Additional information when using a nebuliser:
Cleaning of all nebuliser equipment is essential and should be done daily to prevent infection. See manufacturer’s instructions for the correct procedure for each device.
Cleaning all PARI nebulisers and accessories:
Autoclavable to 136°Celsius
Dish washable
Can be sterilised in boiling water
Can be sterlised in a steam steriliser
Cleaning the SideStream nebulisers:
Wash after every use with warm soapy water
Each week, boil for 10 minutes with a few drops of liquid detergent
Nebulisers should be serviced regularly and parts replaced as per the manufacturers’ instructions. A sign that replacement may be required is if it takes significantly longer to nebulise the solution.
If antibiotics are nebulised, it is advisable to either use a filter attached to the nebuliser, which will absorb over 90% of exhaled antibiotics, or use the device in a well ventilated room, for example, next to an open window (PARI_Filter_Set_instructions). Consideration should also be given to wearing goggles over the eyes when nebulising antibiotics.
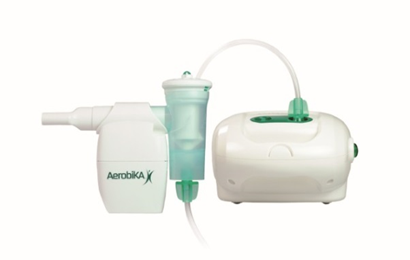
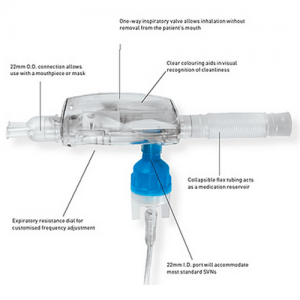
Adding PEP devices to nebulisers (Figs 5-9):
Patients may choose, or be advised, to add positive expiratory therapy to the nebuliser to save time. There is insufficient research to recommend this practice. It may be appropriate for patients with poor adherence to therapy or who are on multiple nebulised medications (Olsen 2015).
In patients with mucus plugging and lobar collapse the combination of PEP therapy and isotonic or hypertonic saline may result in effective mobilisation of mucus.
Do not use PEP with inhaled antibiotics as the addition of PEP significantly decreases the deposition of aerosol within the lungs (Laube 2005).


For information on where to purchase nebulisers’ in Australia and New Zealand – see Resources section.








