Manual techniques apply external forces against the chest wall to facilitate airway clearance when a patient is in a modified or traditional gravity assisted drainage position.
These techniques include:
Chest percussion / clapping
Vibrations
Chest shaking
Percussion
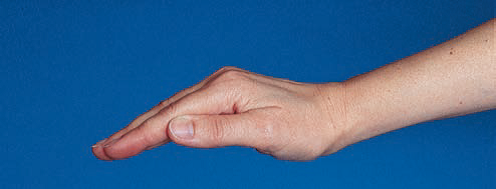
Percussion is performed with a cupped hand to enhance the effect of the technique and the comfort for the patient (Fig 1). The technique, usually performed with two hands (depending on the size of the area), involves the rhythmical
Percussion is performed with a cupped hand to enhance the effect of the technique and the comfort for the patient (Fig 1). The technique, usually performed with two hands (depending on the size of the area), involves the rhythmical flexion and extension of the wrist onto the chest wall at a rate and pressure that is comfortable for the patient (see Manual Techniques video).
The patient may be instructed to do tidal volume breaths or sets of thoracic expansion exercises followed by breathing control. Ideally there should be pauses after 20-30 seconds of continuous percussion and vibrations applied intermittently.
Care must be taken to percuss over the lungs and not over the spine, the clavicles or the sternum and to cover the area to be treated with a towel or thin layer of clothing.
Percussion may also be applied using a mechanical percussor. For infants it may be performed with two or three fingers, an electric tooth brush or a small soft rubber face mask. Both manual and mechanical percussion have equal effects (Bauer 1994).
The rationale for the technique is that the application of force to the chest wall alters the intrapleural pressure. This pressure change is transmitted through to the lung tissue and assists in dislodging secretions from the airway wall.
Following a session of percussion, which may vary from 5 to 15 minutes depending on the condition of the patient, secretions are cleared using expiratory manoeuvres such as the forced expiratory technique (FET) and coughing (see FET video).
Vibrations
Vibration to the chest wall is the manual application of fine oscillatory movements, of high frequency, with chest compression timed with expiration. While vibration is being administered, the patient is instructed to take slow deep breaths (thoracic expansion exercises) to enhance the effect of airflow on the movement of secretions.
The physiotherapist, or family member, places their hands on the patients’ chest, either one hand on top of the other, or side by side, depending on the size of the chest wall. As the patient breathes out, a rapid oscillatory movement is applied in the direction of the normal movement of the ribs and is transmitted through the chest using body weight.
This technique is often combined with the active cycle of breathing (ACBT) and gravity assisted drainage positions to gain more effect.
Vibrations should not be uncomfortable as any discomfort will inhibit expiration and air flow.
Shaking
Shaking is performed in the same manner as vibrations but as a coarse movement. The oscillations are of a larger amplitude and lower frequency than vibrations.
The choice between vibrations or shaking may depend on:
the age and health status of the patient
the clinical experience of the therapist
the use of adjunct techniques
Advantages of manual techniques
Passive treatment option when patient is either too unwell or cognitively not capable of co-operating with more active airway clearance strategies such as positive expiratory pressure (PEP) therapy and huffing
Infants who are not old enough to co-operate with voluntary breathing strategies
Can be applied in intensive care to enhance secretion movement during hyperinflation manoeuvres
Disadvantages of manual techniques
Require a therapist or family member to administer
Can be uncomfortable
Has been shown to cause an increase in hypoxaemia (Falk et al 1984)
May induce bronchospasm in patients with hyper-reactive airways
Contra-indications / precautions for manual techniques
Osteoporosis
# ribs / rib pathology
Thoracic / cardiac surgery
Pain
Frank haemoptysis
Bronchospasm
Liver disease, coagulopathies, BMD deficiency
Metastatic deposits
Clotting disorders
Loss of skin integrity (surgery, burns, wounds)
Subcutaneous emphysema
Evidence
There is limited evidence that manual techniques enhance airway clearance in non-CF bronchiectasis.
In patients with clinically stable cystic fibrosis percussion offers little additional benefit beyond thoracic expansion exercises (Webber 1985) but in patients with non-CF bronchiectasis, secretion clearance was increased (Mazzocco 1985). On the other hand, using vibrations, there was no additional advantage in secretion clearance in non-CF bronchiectasis (Sutton 1985). When applied as a long-term treatment strategy for patients admitted with an acute exacerbation of COPD, no gain in quality of life or fewer number of admissions was associated with the addition of manual techniques compared to ACBT alone.
For patients with COPD who are acutely unwell, percussion has been associated with oxygen desaturation (Connors 1980, Falk 1984) and increased airflow obstruction (Campbell 1975). No adverse effects were noted in patients with non-CF bronchiectasis (Mazzocco 1985).
To minimise side effects, it may be important to incorporate periods of breathing control with percussion in patients who are acutely unwell and to monitor oxygen saturations during treatment.
The clinical application of manual techniques should be directed by the patients’ status, their need for assistance in clearing secretions and the potential for side effects. If the patient finds the technique clinically effective and there are no adverse effects, it can be continued.








