Sputum
It is desirable for children and adults to learn how to expectorate sputum from their lungs to:
document microbiology
direct antibiotic treatment
assist with the monitoring of the condition
If possible, several sputum samples should be collected at baseline followed by 3 to 6 monthly samples.
Purulent sputum reflects neutrophil influx into the secretions. For this reason, the purulence of sputum can be used as a guide to the presence of infection. It not only reflects the likelihood of identifying bacteria but also the bacterial load, the inflammation and damaging potential of the secretions.
During bacterial exacerbations new, or an increased number, of bacteria are found in secretions and this is associated with the production of a key neutrophil chemoattractant (LTB4), necessary to drive neutrophil influx. The release of LTB4 is very dependent upon the bacterial load (which probably explains why patients can be “colonised” by bacteria but remain well). As bacterial numbers rise the neutrophils in the lung also rise, changing the colour of sputum (Stockley et al 2001).
Common microbial isolates from patients with bronchiectasis are:
Haemophilus influenzae (one of the most common bacteria in non-CF bronchiectasis – and more common in younger patients)
Pseudomonas aeruginosa (found in approximately 30% of cases)
Streptococcus pneumoniae
Staphylococcus aureus
Aspergillus fumigatus
(Aksamit et al 2017, McDonnell MJ et al 2015, Finch S et al 2015)
The presence of pseudomonas aeruginosa is associated with increased mortality, increased hospitalisation, more frequent exacerbations, decreased lung function, higher volumes of sputum, more advanced disease on HRCT and a poorer quality of life.
Pathogens analysed from a sputum sample are generally required for the appropriate prescription of medications.
To assist with the monitoring of the condition Murray et al developed a sputum colour chart (Fig. 1).
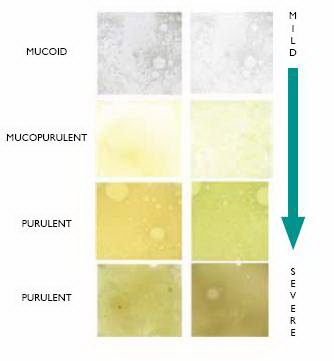
Red due to fresh blood
Brown due to old blood
Grey/black from nicotine and pollution
