Exercise for children
Exercise or physical activity is one of the cornerstones of healthy living in the general population and especially in people with bronchiectasis.
The national guidelines for physical activity and sedentary behaviour are a good starting place for conversations about exercise, to assist the development of an individualised physical activity program.
Many children with mild bronchiectasis may have minimal activity limitation, and should be able to participate in vigorous sports and games with few adaptations. The exercise prescription for children with bronchiectasis will depend on their age and clinical status.
Exercise should include:
cardiovascular and endurance training
muscle strengthening
mobility exercises
The exercise prescription for children with bronchiectasis will depend on their age and clinical status.
Toddlers and young children should always have some form of fun physical activity incorporated into their physiotherapy time. Acceleration activities – eg bouncing on a therapy ball, “flying”, are used in young children to create changes in airflow and volume via external rather than self-generated forces (Fig 1).
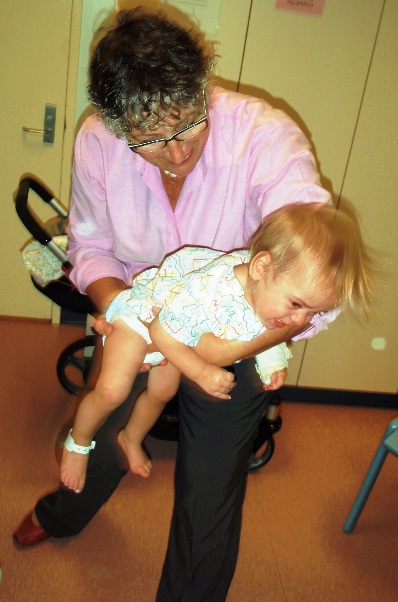

Fig 1 Acceleration activities: Manual acceleration activities can be used in younger children and high
velocity bouncing on therapy ball to create changes in airflow as part of therapy.
The practicality of organising an airway clearance session with an active toddler often means that physical activity is interspersed with other techniques to promote mucus clearance – in this case, “footy”, chasing, and chest percussion intervals of 1-2 minutes with a timer to cue the child and parent (Fig 2).


Fig 2 Chasing and chest percussion
Activities such as “wheelbarrows” and “boxing” games incorporate upper body strengthening and stretching in an age-appropriate, fun and therapeutically valuable way (Fig 3).


Fig 3 Boxing and wheelbarrow activities
Prescription of Exercise
Cycles of exercises, at a moderate intensity, can be utilized as the basis of airway clearance therapy, for children of all ages, if interspersed with the forced expiration technique, assisted autogenic drainage, autogenic drainage or positive expiratory pressure therapy.
When exercises are carried out in different positions (such as upright, side lying, supine or prone) the effects of gravity on regional functional residual capacity and regional ventilation can be utilised.
Physical exercise may be performed before or after airway clearance therapy. Some children perceive that sputum is more easily expectorated if the sputum is loosened with the air flow of exercise prior to their airway clearance session.
A treatment session should always end with physical exercise or at least thoracic expansion exercises, to finish the session with the airways as open as possible.
Examples of exercise programs:


Benefits:
For toddlers, children and adolescents it is a stimulating airway clearance alternative that allows siblings, parents and friends to take an active part
Carrying out physical exercise as the basis of the daily airway clearance therapy constitutes time efficient therapy
The different exercises are easily replaced with new ones, when needed or for variety
The exercises used during each treatment cycle, morning or afternoon treatment sessions, should be varied and this should help to maintain adherence to the treatment
You do not need expensive equipment or large spaces, utilise what is available
Improves quality of life and general well being
Weight bearing exercises increase bone mineral density
Increase socialisation with peers at crèche/school
Tips for exercise
Some patients may benefit from bronchodilators before exercise
Include family members or friends during exercise sessions
Ensure adequate drinking of water before, during and after exercise
Warm up and cool down exercises are essential to effective exercise
Wear appropriate footwear and clothing
Include breathing control or other airway clearance manoeuvres to enhance the effect of exercise
Make exercise fun and enjoyable to gain the interest and participation of the child
Some children or adolescents with more severe lung disease may require supplemental oxygen during exercise periods
Good nutrition is part of the ability to exercise effectively
Evidence for the clinical application of exercise
The inclusion of exercise into airway clearance therapy can aid sputum clearance. There is some evidence that structured exercise programs for people with cystic fibrosis improves fitness, increases thoracic mobility, maintains bone mineral density and preserves or slows the rate of pulmonary decline.
For this reason it is recommended that all patients should be encouraged to exercise several times per week. Exercise programs have also been reported to have beneficial effects both during admissions for acute exacerbations, and in the stable outpatient.








